Moles / Mole Mapping
 Moles are small collections of the normal skin pigment cells called melanocytes. Normally the melanocytes are evenly distributed throughout the skin, but moles are formed when several of the melanocytes are grouped together. Sometimes they are present at birth, but usually they develop as we age. Most people acquire the majority of their moles by the age of 40 and it is rarer to develop new moles after this age. Most moles are brown in colour, ranging from light brown to deeper brown or almost black, but some moles, particularly on the face, are flesh-coloured. They can either be flat or raised.
Moles are small collections of the normal skin pigment cells called melanocytes. Normally the melanocytes are evenly distributed throughout the skin, but moles are formed when several of the melanocytes are grouped together. Sometimes they are present at birth, but usually they develop as we age. Most people acquire the majority of their moles by the age of 40 and it is rarer to develop new moles after this age. Most moles are brown in colour, ranging from light brown to deeper brown or almost black, but some moles, particularly on the face, are flesh-coloured. They can either be flat or raised.
Harmless (benign) moles are very common and most people have at least one or two moles.
For additional information about moles and mole removal options, please explore the sections below and/or contact us today to book an appointment at Dermatology Consulting.
Explore Topics On This Page
Are moles dangerous?
Most moles are completely harmless (benign). Occasionally however some of the pigment cells (melanocytes) in the moles can turn cancerous and develop into a form of skin cancer called melanoma. Melanoma, like most cancers, can be life-threatening, but if it is caught early and removed, it can be cured. However melanoma can also occur as a new development even in normal looking skin so any new brown mark that develops should be checked by a doctor, particularly if it continues to change in shape, outline and pigmentation pattern.
What are the signs a mole is cancerous?
Signs that a mole may be developing into a melanoma are changes in size, shape, colour (including loss of colour) or change in the pattern of pigmentation. Bleeding and itching for no obvious cause, or a white halo developing around the mole can also suggest a suspicious change in the mole.
Melanomas, in fact, can develop not only within moles, but in normal skin, so any new brown spot or lump that develops and shows signs of changing should be assessed.
Very occasionally a melanoma can lose all its pigmentation and be pink (when it is is called an “amelanotic melanoma”), This is rare, but any unusual new skin lesion that is growing or changing should be checked out.
What should be done if a mole is thought to be changing?
If you are concerned about changes in a mole you should seek the advice of a dermatologist, or your general practitioner who can refer you on to a dermatologist if he/she feels it is appropriate. The dermatologist will examine the mole, sometimes under an ordinary magnifying light, and sometimes using a special magnifying light called a dermatoscope which uses polarised light to show some of the pigment pattern under the skin. If the mole does not show any unusual worrying features it can simply be watched. Photographs can be helpful in monitoring of the mole. If the dermatologist is concerned that there is a possibility that the mole may be melanoma, the dermatologist will arrange to remove it urgently by a simple minor operation under a local anaesthetic and send it for analysis.
What is mole mapping?
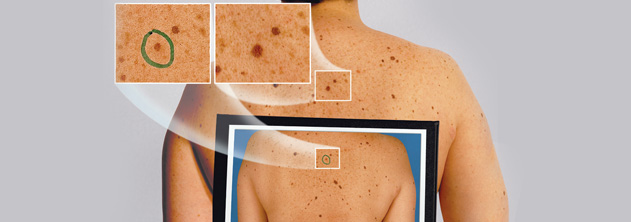 Mole mapping is a photography system documenting the position and appearance of moles. It allows photographs to be taken of the body showing the position of the moles. Following this, close-up photographic images of the appearance of the most unusual moles are taken using a special magnifying light (dermatoscope image). Dermatoscope images are the result of a polarised light shone on to skin and reflected back, which reveals some additional structures and pigment patterns under the skin that are not visible with normal light. These dermatoscope images can be mapped onto the appropriate sites on the body photographs. These photographs then provide a baseline for follow up of the moles to check that they are not changing.
Mole mapping is a photography system documenting the position and appearance of moles. It allows photographs to be taken of the body showing the position of the moles. Following this, close-up photographic images of the appearance of the most unusual moles are taken using a special magnifying light (dermatoscope image). Dermatoscope images are the result of a polarised light shone on to skin and reflected back, which reveals some additional structures and pigment patterns under the skin that are not visible with normal light. These dermatoscope images can be mapped onto the appropriate sites on the body photographs. These photographs then provide a baseline for follow up of the moles to check that they are not changing.
If there are just a few moles of concern these can be photographed by the consultant dermatologist during the consultation. However, if there are many moles this is done by a medical photographer who photographs all the body and maps the magnified dermatoscope images onto the body photographs. It can take a couple of hours to complete.
The role of mole mapping is to provide a baseline image that can be used for future monitoring of the moles. After the photographs are taken, it is suggested that a follow-up visit occurs three months later to compare the moles with the photographs to check the moles are stable. Following that, a plan for future follow up visits can be made if appropriate.
It is important to remember with mole mapping that it is change that is important, so it is important that patients attend for follow up visits if recommended by the consultant dermatologist.
Testimonials
“I have been seeing Dr Farrell for a few years now for various treatments and mole checks. She is thorough and incredibly knowledgeable, she takes her time to explain why skin changes occur and what is done to correct them. I trust her implicitly with all of my , and my families, skin care needs.”


